- Vegans have the highest bone-related risk
- On average, vegans have the lowest bone density
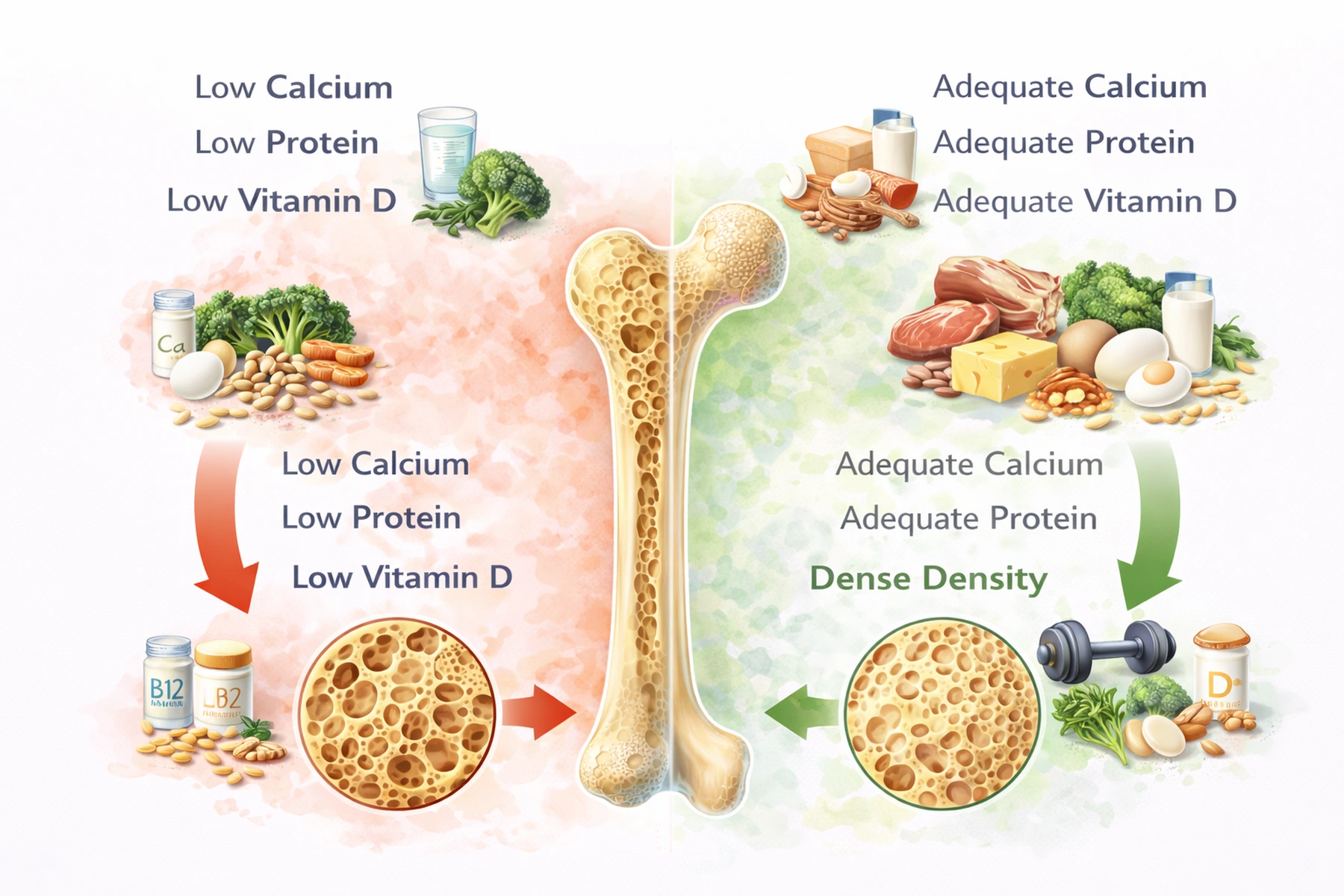
- Calcium and vitamin D are critical
- Protein deficiency lowers IGF-1
- Vitamin K2 supports mineralization
- B12 also matters for bone health
As you may have already understood, the idea of this website is to compare the pros and cons of different eating patterns — meat-eaters, vegetarians, and vegans. In this article, for variety, we will point to a topic where vegans have drawn the short straw, namely bone density and, respectively, bone strength in people following different dietary patterns. The initial comparison is as follows:
Comparison
Omnivores
- Highest average BMD (bone mineral density)
- Lowest fracture risk overall
- Usually consume more calcium, vitamin D, high-quality protein, vitamin K2, B12
- Higher BMI → greater mechanical load → stronger bones
Vegetarians
- Slightly lower BMD than omnivores, but usually still normal
- Fracture risk: moderately higher
- Protein is lower than in omnivores
- Calcium/vitamin D are often adequate if dairy products/eggs are consumed
Vegans
- Lowest BMD on average (the femoral neck and lumbar spine are most affected)
- Highest fracture risk, especially hip fractures
- Major risk factors:
- Low calcium intake
- Low vitamin D
- Lower total protein → lower IGF-1 levels
- Lack of vitamin K2 (found almost exclusively in animal or fermented foods)
IGF-1 is a hormone produced in the liver in response to consuming enough protein and overall calories.
It plays a major role in:
- Bone formation → stimulates osteoblasts
- Muscle growth → anabolic effect
- Cartilage formation
- Growth during childhood
- Healing and regeneration
In simpler words:
IGF-1 is one of the body’s main “building hormones.”
✔ How is it linked to diet?
Higher protein intake → higher IGF-1
Lower protein content (common in poorly planned vegan diets) → lower IGF-1
Vitamin K2 = menaquinone, a form of vitamin K with a special role in bone health.
✔ Purpose of vitamin K2
Vitamin K2 activates a protein called osteocalcin, which is responsible for:
Absorbing calcium and “locking” it into the bone matrix.
Without K2:
- osteocalcin remains inactive
- calcium cannot be used effectively
- bones mineralize poorly
✔ Why vegans often do not get enough K2
K2 is found mainly in:
- Eggs
- Cheese
- Liver
- Butter
- Fermented foods (natto, some fermented cheeses)
Vegans who do not eat natto or take a K2 supplement (MK-7) usually get almost no K2 naturally.
That is why K2 is part of the “bone health optimization” checklist for vegans.
BUT not everything is lost! Well-planned vegan diets can lead to a significant reduction or removal of these disadvantages.
Why does this happen?
After showing that it is not always cool and trendy to be plant-based, it is time to show why, in this aspect, the “bad” people who eat meat have an advantage. In other words, we will trace the biochemical mechanism responsible for the changes that happen in our bones.
Nutritional pathways that affect the cycle
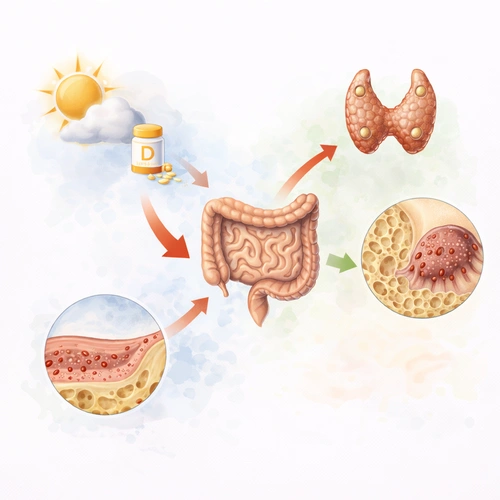
Calcium and vitamin D
- Vitamin D increases calcium absorption in the intestines
- Low D leads to low absorption and the body increases parathyroid hormone (PTH), which increases bone breakdown
Vegans often have lower vitamin D levels → higher PTH → greater osteoclast activity (more bone breakdown).
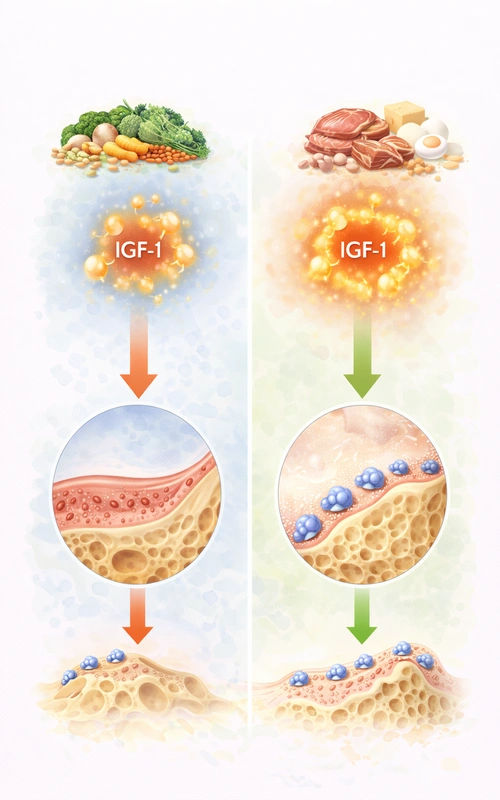
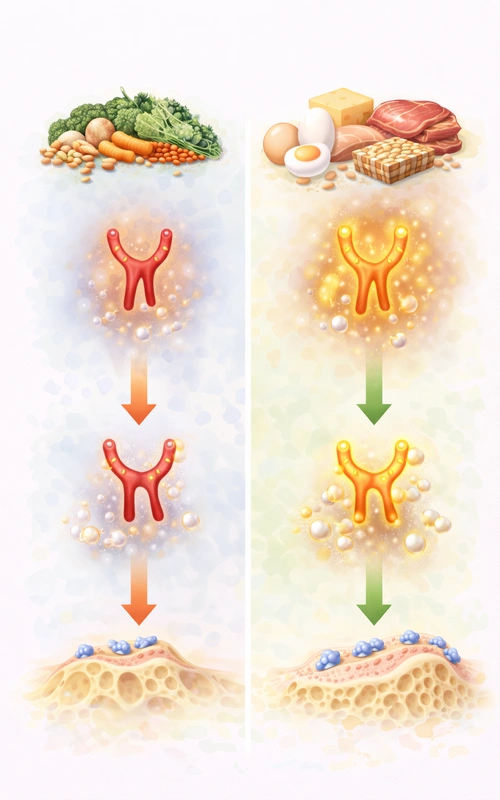
Protein → IGF-1
(explains much of what is happening)
Protein intake stimulates IGF-1, one of the strongest anabolic agents for bones.
- Higher IGF-1 increases osteoblast activity
- Lower IGF-1 reduces bone tissue formation
Vegans tend to have lower serum IGF-1 levels because of:
- Lower total protein
- Lower density of essential amino acids
- Lower availability of leucine and lysine
This explains the reduced osteoblast activity found in some studies
Vitamin K2 (Menaquinone)
K2 activates osteocalcin, the protein that binds calcium to the bone matrix.
K2 is found mainly in:
- dairy products, egg yolks, liver
- some fermented foods
Vegans who do not consume fermented foods have minimal K2 and less activation of osteocalcin, resulting in reduced bone mineralization.
Vitamin B12 and homocysteine
Low B12 → elevated homocysteine → impaired collagen cross-linking → weaker bone microarchitecture.
Body weight and mechanical loading
Heavier people apply greater pressure on the bone, thereby stimulating osteocytes and signaling osteoblasts to build bone. Finally, there is some benefit to being heavy.
Vegans tend to have lower body weight and therefore:
→ less loading
→ less stimulus for bone tissue formation
Phytates
Found in grains, legumes, seeds — they bind calcium, zinc, and iron.
Vegans have a higher phytate content in their diet unless foods are:
- soaked
- sprouted
- fermented
Untreated phytates lead to reduced mineral bioavailability.
Summarized in a table, things look as follows:
Mechanism | Effect on bones | Higher risk in |
Low calcium | Reduced mineralization | Vegans, some vegetarians |
Low vitamin D | High PTH → high resorption (think of it as reverse absorption) | Vegans |
Low protein | low IGF-1 | Vegans |
Low vitamin K2 | low osteocalcin activation | Vegans |
Low vitamin B12 | low collagen quality | Vegans |
Low body weight | low mechanical load | Vegans/vegetarians |
High phytates | low mineral absorption | Vegans |
Ideas
Now that we understand how difficult it is to be a vegan bone these days, it is time to see what the poor people can do so they do not break while getting up from a chair or, imagine this, if they decide to lift heavy objects. Meat-eaters and vegetarians — in this case everything is fine for you; you can move on to the next articles.
List of key nutrients
1. Calcium: 1000–1200 mg/day
Sources:
- Fortified plant milks (THE most reliable source)
- Calcium-set tofu
- Kale, bok choy, broccoli
- Supplements if dietary intake is <800 mg/day
Goal: ≥800 mg/day from diet, supplement the rest.
2. Vitamin D: 1000–2000 IU/day
Since sun exposure is unreliable, and roasting yourself like toast will not help.
Supplements are the simplest, healthiest, and safest option.
3. Protein: minimum 1.0–1.2 g/kg
Higher than the recommended daily intake because plant protein is less anabolic.
Tips:
- Mix plant proteins to get a complete amino acid profile
- Prioritize: soy, tofu, tempeh, seitan, pea protein, legumes
- Include 20–30 g protein per meal
4. Vitamin B12: mandatory
Either:
- 2000 mcg cyanocobalamin weekly
- or 250 mcg daily
5. Vitamin K2
This is a major missing link for vegans.
Options for getting it:
- Natto (fermented soybeans)
- Vegan K2 supplements (MK-7)
6. Omega-3 (EPA/DHA)
Recommended: 250–500 mg/day algae-based EPA/DHA
EPA/DHA reduces inflammation → supports preservation of the bone matrix.
7. Reduce phytates (optional, but useful)
To improve mineral absorption:
- Soak beans
- Sprout seeds
- Use sourdough bread instead of regular bread
- Ferment soy (miso (this is not meat, said with an Eastern accent), tempeh)
Lifestyle habits that matter MOST
Strength training
Stimulates osteoblasts more than any nutrient.
Best exercises:
- Squats
- Deadlifts
- Lunges
- Leg press
- Hip thrusts
- Weighted walking / running
- Jump training (plyometrics)
3–4 workouts per week lead to a huge improvement.
2. Maintain a normal BMI – body mass index
BMI below 19 drastically increases fracture risk.
Goal: BMI 20–25
3. Limit alcohol and avoid smoking
Directly reduces osteoblast function and calcium retention.